Bariatric (metabolic) surgery can succeed where diet after diet has stalled. The minimally invasive procedures reshape your stomach and small intestine so you absorb fewer calories and feel full faster. According to long-term cohort studies, patients shed about 30 percent of their starting weight and keep it off for years on average (pmc.ncbi.nlm.nih.gov). That's a life-changing payoff, yet surgery is still a serious medical decision. This quick guide shows how each option works, who qualifies, and what everyday life looks like after surgery, so you can choose your next step with clarity and confidence.
What is bariatric surgery?
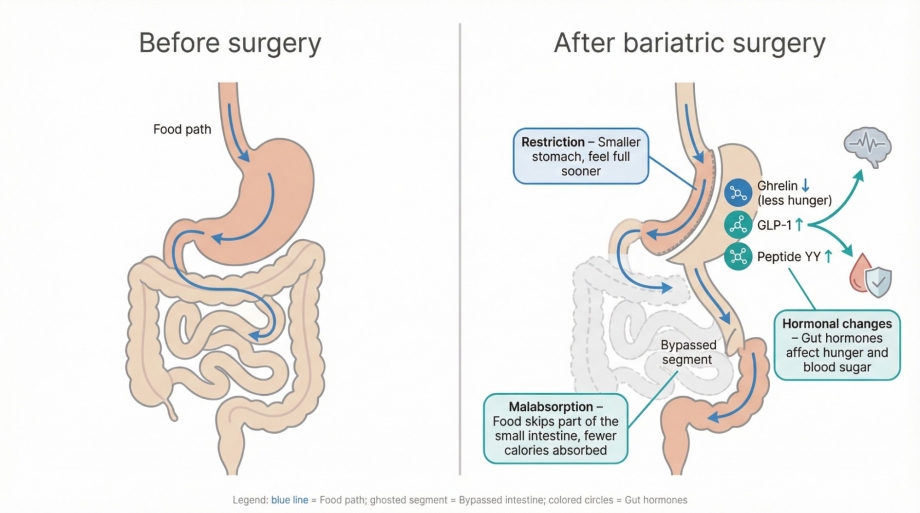
Bariatric (also called metabolic) surgery is the umbrella for procedures such as sleeve gastrectomy and gastric bypass that rebuild the digestive tract to support lasting weight loss. Surgeons use two main tactics: restriction, which creates a smaller stomach so you feel full sooner, and malabsorption, which reroutes part of the small intestine so you absorb fewer calories. Research shows a third metabolic effect as well: the operations lower hunger hormones like ghrelin and raise GLP-1 and peptide YY, improving blood-sugar control even before significant weight loss occurs, according to PubMed.
Clinically, these changes can put type 2 diabetes into remission, reduce long-term mortality, and deliver about thirty percent sustained weight loss on average, according to PubMed. The surgeries are becoming more common—roughly 270 000 Americans chose a metabolic procedure in 2023, yet that is still only around one percent of those who qualify, according to the American Society for Metabolic and Bariatric Surgery (ASMBS). The ultimate goal is larger than a smaller waistline: expect better heart health, steadier energy, and an overall higher quality of life.
Who might be a candidate?
Most programs follow national guidelines. Adults generally qualify when body mass index (BMI) is forty or higher, or thirty-five to 39.9 with a serious condition such as type 2 diabetes or obstructive sleep apnea, according to PubMed. Some centers now consider BMI thirty to 34 in adults with poorly controlled diabetes, and select adolescents may qualify after a multidisciplinary review.
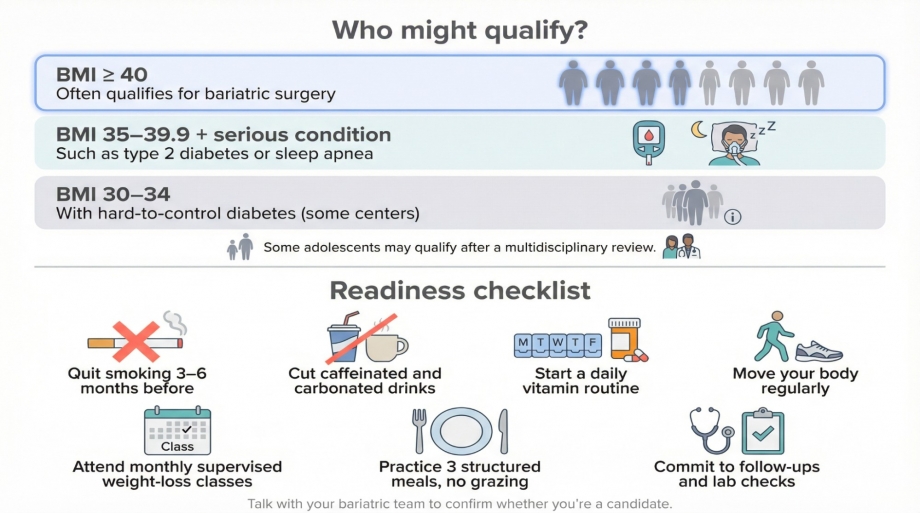
Readiness matters as much as BMI, and most programs will ask you to start changing your habits months before the operation. The Bariatric & Metabolic Center of Colorado's bariatric surgery guide notes that patients must quit smoking three to six months before the operation and attend monthly medically supervised weight-loss classes for six months. These pre-surgery guidelines also recommend cutting out caffeinated and carbonated drinks, practicing three structured meals a day without grazing, and beginning a daily vitamin routine well before surgery. Surgery tends to succeed when you:
- Adopt protein-focused meals and mindful portions
- Move your body regularly in ways you enjoy
- Attend follow-up visits and routine lab checks
- Take prescribed vitamin and mineral supplements every day
Although about twenty million United States adults meet the BMI criteria, fewer than one percent pursue metabolic surgery each year, according to ASMBS. Awareness, insurance coverage, and personal preference all influence that gap.
Common types of bariatric surgery
About 270 000 metabolic procedures took place in the United States in 2023. Roughly sixty percent were sleeve gastrectomies and about twenty-five percent were Roux-en-Y gastric bypasses. No single operation is best for everyone, because each balances weight-loss potential, complication risk, and lifestyle fit. The next sections outline how the leading options work and why your team may recommend one over another.
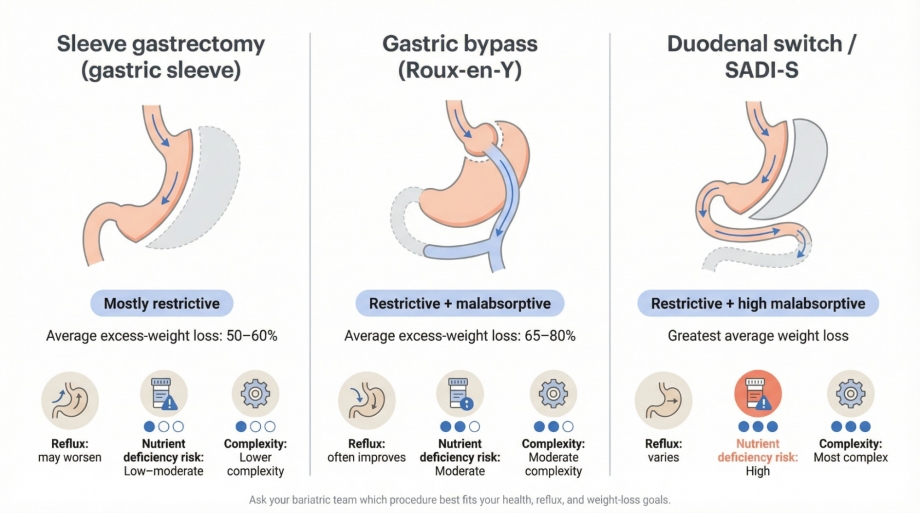
Gastric sleeve (sleeve gastrectomy)
During a sleeve gastrectomy, surgeons remove roughly seventy-five percent of the stomach, leaving a narrow tube shaped like a banana. The smaller reservoir limits meal size and sharply lowers the hunger hormone ghrelin, so appetite often declines early on. Sleeve surgery accounts for about fifty-eight percent of all United States metabolic procedures, or roughly 157 000 operations in 2023, according to ASMBS.
What to expect: large cohort studies show fifty to sixty percent excess-weight loss two years after surgery, with durable results at five years for many participants, according to PubMed. Diabetes remission and lower blood pressure are common benefits. New or worsening acid reflux can occur, so sleeve surgery is not ideal for everyone. Your care team weighs simplicity and shorter operative time against reflux risk and slightly less weight loss than gastric bypass before advising.
Gastric bypass (roux-en-y)
Roux-en-Y gastric bypass creates a thumb-sized stomach pouch and routes food around the first three to four feet of small intestine. The pouch restricts intake, while the shortcut reduces calorie absorption and triggers hormonal shifts that improve blood-sugar control.
Although the sleeve now dominates, about 63 000 Americans chose gastric bypass in 2023, or one procedure in four, according to ASMBS. Average excess-weight loss reaches sixty-five to eighty percent within two years, the highest among mainstream surgeries, according to PubMed. A 2024 meta-analysis reports that roughly sixty percent of people with type 2 diabetes enter remission after bypass, with lower long-term relapse than after sleeve surgery, according to PubMed.
Bypass often relieves severe reflux but carries higher risks of vitamin-mineral deficiencies and “dumping” symptoms when meals are high in sugar. Your team balances durable weight loss and strong metabolic impact against a more complex operation and lifelong supplement needs before recommending bypass.
Other procedures
Roughly one percent of patients choose duodenal switch–style operations, including single-anastomosis duodenal switch (SADI-S). These combine a sleeve gastrectomy with an extensive intestinal bypass and deliver the greatest average weight loss, yet they demand strict nutrient monitoring because malabsorption is high, according to ASMBS.
Revisional surgery is rising as earlier gastric bands or sleeves need adjustment; it made up about seventeen percent of United States metabolic procedures in 2019 and continues to grow. Endoscopic tools now allow some revisions or primary treatments, such as intragastric balloons or endoscopic sleeve gastroplasty, without new incisions. Durability is typically lower and insurance coverage varies.
Your team may recommend one of these less common paths if you have significant weight to lose after a prior surgery, severe metabolic disease, or anatomical issues such as persistent reflux or a stretched sleeve. The decision weighs added weight-loss power against higher nutrient-deficiency risk, operative complexity, and coverage limits.
How safe is bariatric surgery?
Today's metabolic procedures have a thirty-day mortality rate of about 0.1 percent and a major-complication rate near four percent, similar to or lower than gallbladder removal or knee replacement, according to ASMBS. Advances in laparoscopy, anesthesia, and enhanced recovery protocols have driven this progress over the past two decades.
Complications can still occur. The most serious include bleeding, infection, or blood clots in the first days after surgery; staple-line leaks during the first week; and long-term nutrient deficiencies if supplements or lab checks lapse. Your bariatric team mitigates these risks by screening individual factors, giving preventive blood thinners, performing leak tests, and monitoring you closely after discharge.
Why consider any risk? Severe obesity doubles or triples the chances of dying from heart disease, stroke, or diabetes. Large cohort studies show that metabolic surgery lowers all-cause mortality by up to forty percent over ten years, according to ASMBS. For many people, treating the disease outweighs the small procedural risk.
Life after bariatric surgery
Think of surgery as mile one of a marathon, not the finish line. In the first six weeks most programs guide you through four eating phases: clear liquids, full liquids with protein shakes, soft-blended foods, and a gradual return to regular textures. By week eight most people can tolerate nearly all foods again, but portions stay small—a few ounces—with protein in the spotlight. You will sip water steadily, about 48–64 ounces per day, to stay hydrated and begin a daily vitamin and mineral routine that continues for life.

What changes can you expect? Studies show that physical-health scores on the SF-36 survey rise from an average of 34 to 46 in six months and 50 at two years, while mental-health scores climb by about ten points in the same period, according to PubMed. More than one-half of participants see obstructive sleep apnea resolve or improve substantially, according to PubMed. Knee-pain research also reports meaningful relief that lasts at least five years, according to PubMed.
Alongside these gains come new habits: moving your body most days, attending follow-up appointments and annual lab checks, and leaning on support groups or counseling when emotions around food or body image surface. People who stay engaged with their care team keep more long-term weight off and report higher life satisfaction, proof that the journey is ongoing yet well worth the effort.